Breast reduction
Reduction mammoplasty; Macromastia - reductionBreast reduction is surgery to reduce the size of the breasts.
Description
Breast reduction surgery is done under general anesthesia. This uses medicines that keep you asleep and pain-free.
General anesthesia
General anesthesia is treatment with certain medicines that puts you into a deep sleep-like state so you do not feel pain during surgery. After you ...
Read Article Now Book Mark ArticleFor a breast reduction, the surgeon removes some of the breast tissue and skin. Your nipples may be moved higher to reposition them for cosmetic reasons.
In the most common procedure:
- The surgeon makes three surgical cuts (incisions) around the areola (the dark area around your nipples), from the areola down to the crease under your breast, and across the lower crease of your breast.
- Extra fat, skin, and breast tissue are removed. The nipple and areola are moved to a higher position. Often the areola is made smaller.
- The surgeon closes the cuts with stitches to reshape the breast. The stitches may be dissolvable or removed later.
- Sometimes liposuction is combined with breast reduction to improve the shape of the breast and armpit areas.
Liposuction
Liposuction is the removal of excess body fat by suction using special surgical equipment. A plastic surgeon typically does the surgery.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
The procedure can last 2 to 5 hours.
Why the Procedure Is Performed
Breast reduction may be recommended if you have very large breasts (macromastia) and:
- Chronic pain that affects your quality of life. You may be having headaches, neck pain, or shoulder pain.
- Chronic nerve problems caused by poor posture, which result in numbness or tingling in your arms or hands.
- Cosmetic problems, such as persistent bra-strap groove, scar-like lines in the skin (striae), difficulty finding clothes that fit, and low self-confidence.
- Chronic rashes under your breasts.
- Unwelcome attention that is making you feel awkward.
- Inability to participate in sports.
Some women may benefit from non-surgical treatments, such as:
- Exercising to strengthen their back and shoulder muscles
- Losing excess weight
- Wearing supportive bras
Risks
Risks of anesthesia and surgery in general are:
- Reactions to medicines
- Breathing problems
Breathing problems
Breathing difficulty may involve:Difficult breathing Uncomfortable breathingFeeling like you are not getting enough air
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Bleeding, blood clots, or infection
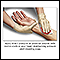
Bleeding
Bleeding is the loss of blood. Bleeding may be:Inside the body (internal)Outside the body (external)Bleeding may occur:Inside the body when blood le...
 ImageRead Article Now Book Mark Article
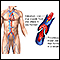
ImageRead Article Now Book Mark ArticleBlood clots
Blood clots are clumps that occur when blood hardens from a liquid to a solid. A blood clot that forms inside one of your veins or arteries is calle...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Risks of this procedure are:
- Difficulty breastfeeding, or being unable to breastfeed
- Large scars or wounds that take a long time to heal
- Loss of feeling in the nipple area
- Uneven position of the nipples or differences in the size of the breasts
Before the Procedure
Ask your surgeon if you need a screening mammogram based on your age and risk of having breast cancer. This should be done long enough before surgery so if more imaging or a biopsy is needed, your planned surgery date won't be delayed.
Tell your surgeon or nurse if:
- You are or could be pregnant.
- You are taking any medicines, including medicines, drugs, supplements, or herbs you bought without a prescription.
Planning for your surgery:
- If you have diabetes, heart disease, or other medical conditions, your surgeon may ask you to see your health care provider who treats you for these conditions.
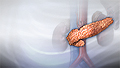
Diabetes
Diabetes is a long-term (chronic) disease in which the body cannot regulate the amount of sugar in the blood.
 ImageRead Article Now Book Mark Article
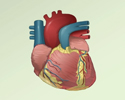
ImageRead Article Now Book Mark ArticleHeart disease
Coronary heart disease is a narrowing of the blood vessels that supply blood and oxygen to the heart. Coronary heart disease (CHD) is also called co...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - If you smoke, it's important to cut back or quit. [Smoking can slow healing and increase the risk for complications. Your surgery may be delayed if you don't stop. Ask your provider for help quitting smoking.
Quitting smoking
There are many ways to quit smoking. There are also resources to help you. Family members, friends, and co-workers may be supportive. But to be su...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - If needed, prepare your home to make it easier to recover after surgery.
Prepare your home
Getting your home ready after you have been in the hospital often requires much preparation. Set up your home to make your life easier and safer when...
Read Article Now Book Mark Article - Ask your surgeon if you need to arrange to have someone drive you home after your surgery.
During the week before your surgery:
- You may be asked to temporarily stop taking medicines that keep your blood from clotting. These medicines are called blood thinners. This includes over-the-counter medicines and supplements such as aspirin, ibuprofen (Advil, Motrin), naproxen (Aleve, Naprosyn), and vitamin E. Many prescription medicines are also blood thinners.
- Ask your surgeon which medicines you should still take on the day of the surgery.
On the day of surgery:
- Follow instructions about when to stop eating and drinking.
- Take the medicines your surgeon told you to take with a small sip of water.
- Arrive at the hospital on time.
After the Procedure
You may go home the same day or stay overnight in the hospital.
A gauze dressing (bandage) will be wrapped around your breasts and chest. Or, you will wear a surgical bra. Wear the surgical bra or a soft supportive bra for as long as your surgeon tells you to. This will likely be for several weeks.
Drainage tubes may be attached to your breasts. These tubes will be removed within a few days.
Your pain should decrease in a few weeks. Ask your surgeon if you can take acetaminophen (Tylenol) or ibuprofen (Advil) to help with pain instead of a narcotic medicine. If you do use a narcotic medicine, be sure to take it with food and plenty of water. Do not apply ice or heat to your breasts unless your surgeon has told you that is OK.
Ask your surgeon when it is OK to shower or bathe.
Within a few weeks, the swelling and bruising around your incisions should disappear. You may have a temporary loss of sensation in your breast skin and nipples after surgery. Sensation may gradually return over time.
Follow any other self-care instructions you are given.
Self-care instructions
You had cosmetic breast surgery to change the size or shape of your breasts. You may have had a breast lift, breast reduction, or breast augmentatio...
Read Article Now Book Mark ArticleSchedule a follow-up visit with your surgeon. At that time you will be checked for how you are healing. Sutures (stitches) will be removed if needed.
Outlook (Prognosis)
You are likely to have a very good outcome from breast reduction surgery. You may feel better about your appearance and be more comfortable with various activities.
Pain or skin symptoms, such as striation, may disappear. You may need to wear a special supportive bra for a few months for comfort and to help with healing.
Scars are permanent. They will be more visible for the first year, but will then fade. The surgeon will make every effort to place the surgical cuts so that scars are hidden. Cuts are usually made on the underside of the breast and around the areola. Most of the time, the scars should not be noticeable, even in low-cut clothing. Your surgeon will give you instructions on how to care for your scars.
References
American Board of Cosmetic Surgery website. Breast reduction guide. www.americanboardcosmeticsurgery.org/procedure-learning-center/breast/breast-reduction-guide/. Accessed February 24. 2025.
Hall-Findlay E, Bolletta E, Muñoz Ledo GJ. Short scar breast reduction. In: Nahabedian MY, Neligan PC, eds. Plastic Surgery: Volume 5: Breast. 5th ed. Philadelphia, PA: Elsevier; 2024:chap 8.
Mammoplasty - illustration
Mammoplasty is a common surgical procedure to change the size of the breasts. Mammoplasty may also be done when the breasts are markedly different in size.
Mammoplasty
illustration
Review Date: 2/17/2025
Reviewed By: David A. Lickstein, MD, FACS, specializing in cosmetic and reconstructive plastic surgery, Palm Beach Gardens, FL. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.


